Minimally Invasive Spine Surgery (MIS)
Minimally Invasive Spine Surgery (MIS) is a cutting-edge approach that treats spinal conditions through small incisions using advanced imaging and surgical tools. This technique allows your surgeon to access and repair damaged spinal structures without disturbing surrounding healthy tissues. MIS is often used to treat herniated discs, spinal stenosis, spinal instability, and other degenerative conditions.
Unlike traditional open surgery, MIS significantly reduces muscle disruption, postoperative pain, and healing time—helping patients get back to their lives sooner and with fewer complications.
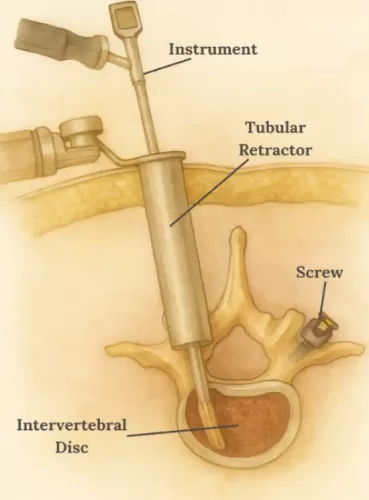
How It Works
MIS procedures are performed through tiny incisions, often less than an inch long. Using specialized instruments and real-time imaging (such as fluoroscopy or surgical microscopes), your surgeon can visualize the spine and precisely address the problem area.
Whether it involves removing herniated disc material, decompressing pinched nerves, or stabilizing vertebrae with screws and rods, MIS allows the same surgical goals to be met as with open surgery—but with minimal tissue damage.
Some common MIS procedures include:
- Microdiscectomy
- Laminectomy
- Spinal fusion (minimally invasive)
- Decompression for spinal stenosis
Because of the precision involved, MIS generally results in less blood loss, shorter operative times, and reduced hospitalization compared to traditional techniques.
Conditions Treated
- Herniated or bulging discs
- Spinal stenosis (narrowing of the spinal canal)
- Degenerative disc disease
- Spondylolisthesis (slippage of one vertebra over another)
- Spinal instability
- Chronic lower back or neck pain not responsive to conservative treatment
- Sciatica or nerve compression
- Spinal fractures (in select cases)
Frequently Asked Questions (FAQs)
Is Minimally Invasive Spine Surgery safe?
Yes. MIS is performed by trained spine surgeons using precise, image-guided techniques. It is considered safe and effective for many spinal conditions, with fewer complications compared to open surgery.
How long is the recovery?
Many patients return home the same day or after a short hospital stay. Full recovery varies by procedure and individual but is typically faster than with open surgery—often within 4–6 weeks.
Is MIS painful?
Most patients report less postoperative pain than traditional surgery due to reduced tissue disruption. Pain is typically managed with medications and a gradual return to activity.
Will I need physical therapy?
Yes. Postoperative rehabilitation is an important part of recovery to restore mobility and strength. Your care team will customize a therapy plan based on your procedure and condition.
Is MIS right for everyone?
Not all patients are candidates for MIS. Your doctor will evaluate your condition, imaging, and health history to determine if you qualify for this approach.
What Types of Results Can I Expect from MIS?
Many patients experience:
- Significant reduction in pain and numbness
- Improved mobility and activity level
- Quicker return to work or daily activities
- Lower risk of postoperative complications
- Minimal scarring and cosmetic concerns
Results depend on the condition treated, the extent of damage, and patient commitment to post-op care. With the right plan, MIS can dramatically improve quality of life.
Mayo Clinic. (2023). Minimally Invasive Spine Surgery Overview. Retrieved from https://www.mayoclinic.org
American Association of Neurological Surgeons (AANS). (2023).
MIS Techniques and Benefits. Retrieved from https://www.aans.org
National Institute of Neurological Disorders and Stroke (NINDS). (2023).
Spinal Surgery and Neuromodulation. Retrieved from https://www.ninds.nih.gov